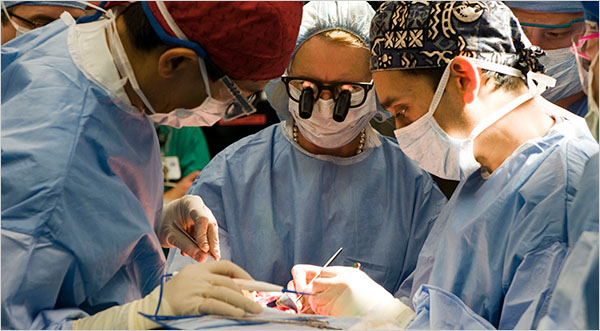
Dr. Maria Siemionow, center, led a Cleveland Clinic team including Dr. Risal Djohan, left, and Dr. Daniel Alam in an operation replacing most of a patient’s face. Cleveland Clinic, via Associated Press
CLEVELAND – Only the forehead, upper eyelids, lower lip, lower teeth and jaw are hers.
The rest of her face comes from a cadaver.
In a 23-hour operation, transplant surgeons have given nearly an entire new face to a woman with facial damage so severe that she could not eat on her own or breathe without a hole in her windpipe, doctors at the Cleveland Clinic said here on Wednesday.
The highly experimental procedure, performed within the last two weeks, was the world’s fourth partial face transplant, the country’s first, and the most extensive and complicated such operation to date. Dr. Maria Siemionow led the surgical team, which took turns at the operating table so the doctors could rest, sleep and share expertise.
The woman’s identity was not disclosed, nor was the cause of her injury or the donor’s identity.
The woman is eventually expected to eat, speak and breathe normally and even smell again, her doctors said at a news conference. Feeling should return to her face in six months, and most facial functions in about a year, leading to her ability to smile after physical therapy to help train the muscles for that function.
But because facial structure varies among people, the woman is not expected to look like her donor, the doctors said.
The woman will need to take antirejection drugs for the rest of her life, but those drugs do not guarantee success. Although rejection reactions seem more common in the first few months, they can occur at any time. Doctors can often reverse such reactions by adjusting the drug regimen.
The woman has cleared the earliest hurdle: she has not rejected the new face. The doctors said she was doing well but emphasized that they could not predict the future, as she faces potential complications like infections and cancers resulting from the immunosuppression treatment.
The clinic team said that if the transplant ever failed, it would be replaced with a skin graft taken from parts of the woman’s body.
The woman needed the transplant because of severe functional loss from trauma. She could breathe only through a hole in her windpipe because of scarring from the trauma and earlier reconstructive surgery.
Surgeons have performed multiple reconstructive procedures over the several years that the woman has been under their care, the doctors said, adding that they were left with no conventional treatment options to restore her facial function.
“Our patient was called names and was humiliated,” Dr. Siemionow said. “Children ran away.”
She added, “You need a face to face the world.”
The operation was fiendishly complex, the doctors said. They had to integrate functional components like a nose and lower eyelids, as well as different tissue types, including skin, muscles, bony structures, arteries, veins and nerves. About 77 square inches of tissue were transplanted from the donor.
“This is not cosmetic surgery in any conventional sense,” said Dr. Eric Kodish, chairman of the clinic’s bioethics department, who was part of the team that interviewed and evaluated the patient’s understanding of the risks in the experimental procedure.
Dr. Kodish said that in psychological testing she was asked questions like these: Is it you or someone else in your family who wants you to have the face transplant? How do you feel about the prospect of living with a face from a dead person?
Under the clinic’s scientific blueprint, Dr. Kodish said, the patient was not allowed to see a photo of the donor, in part because it could lead her to believe she would look like the donor.
The trauma cost the woman sight in her right eye, and vision from the left eye is impaired. Before the transplant, she could make out the faces of her doctors.
As she awakened from heavy sedation, Dr. Chad Gordon, a plastic surgeon, said she gave a thumbs-up sign when asked how she was feeling. As she recovers in the clinic, she communicates mostly in writing.
Dr. Siemionow said, “I must tell you how happy she was when with both her hands she could go over her face and feel that she has a nose, feel that she has a jaw.”
Dr. Siemionow, 58, a native of Poland, said she began preparing for the face transplant 20 years ago. Her research has involved transplants on animals and cadavers and ethical concerns.
Along the way, the Royal College of Surgeons in England in 2003 and an ethics committee in France in 2004 said in reports that the risks of the surgery far outweighed the benefits at that time. (The British are now said to be more permissive.)
But in late 2004, a Cleveland Clinic institutional review board said a face transplant was ethical and possible and approved Dr. Siemionow’s scientific blueprint for the experimental procedure. It was the first time any ethics committee in the world had given such permission.
Medical ethicists said Wednesday that in face transplant surgery the risks and benefits to the patient must be weighed carefully.
“Not to downplay the difficulties of having a facial disfigurement, but one can live a long life and be disfigured,” said Stuart G. Finder, director of the Center for Healthcare Ethics at Cedars-Sinai Medical Center in Los Angeles.
But the benefits of a face transplant are not only cosmetic, Dr. Finder said, adding, “The repair of the face can also have significant social consequences – like the ability to speak, or the ability to eat, that can be replaced because of having lips.”
In late November 2005, surgeons performed the world’s first partial face transplant in Amiens, France, on Isabelle Dinoire, 38, who was seriously disfigured by her Labrador retriever.
Meanwhile, Dr. Siemionow worked with organ and tissue recovery organizations for help in finding a donor and interviewed patients who contacted the Cleveland Clinic seeking a face transplant. She said she did not recruit any patients for the transplant.
A major obstacle was finding donors whose sex, race, age and blood type matched that of potential recipients. Specific consent procedures were developed.
About four months ago, the clinic put out a request for a donor because the doctors had exhausted all other treatment options for the woman. When LifeBanc of northeast Ohio identified a donor, it called Dr. Siemionow, who in turn called the other team members from a number of specialties to activate a well-rehearsed drill.
The transplant procedure began at 5:30 p.m. on an unspecified recent day as doctors tried to determine that the arteries and veins in the recipient’s neck, scarred from trauma and earlier surgery, could receive the transplant.
At 8 p.m., surgeons began recovering the donor’s facial tissues, carefully dissecting the arteries, nerves, soft tissue and bones to ensure a good blood supply. That effort took 9 hours, 10 minutes.
Meanwhile, surgeons removed scar tissues from the woman to make room for the facial graft.
At 5:10 the next morning, the surgeons began connecting the patient’s blood vessels to the donor graft vessels. When the graft turned pink and showed no signs of an immediate rejection, they went on to attach the facial graft to the woman’s face. They used microscopes to stitch arteries, veins and nerves from the donor graft to the woman’s head. Her ears and scalp are her own.
By 4:30 p.m., the woman had a new face.
By LAWRENCE K. ALTMAN Published: December 17, 2008
Source: The New York Times